Humanitarian crises—defined as events or series of events that represent a critical threat to the health, safety, security or wellbeing of a community or other large group of people—present unique challenges to maternal and newborn health. In such situations, women and newborns often face increased risk of poor health outcomes due to sudden loss of medical support and inadequate access to sexual, reproductive and maternal health services as well as trauma, malnutrition, disease and gender-based violence.
“Making motherhood safe for women and children is a top priority in humanitarian settings. Every day, around 500 women die in pregnancy or childbirth in humanitarian and fragile settings.” – Massimo Diana, Representative, UNFPA Syria
Weakened health systems and redistribution of limited resources in humanitarian settings may also compromise maternal and newborn health. Furthermore, difficulty collecting accurate data in such settings may hinder responders’ ability to identify and address pressing maternal and newborn health needs.
This three-part series will explore maternal and newborn health issues through the lens of three humanitarian settings, starting with an example of an infectious disease outbreak.
2014 Ebola outbreak in West Africa
The Ebola virus was first discovered in 1976 when there were simultaneous outbreaks in what is now South Sudan and the Democratic Republic of the Congo near the Ebola River. Five different species of Ebola, also referred to as “Ebola hemorrhagic fever,” have been identified. The virus is transmitted from infected animals to humans and can spread to other humans through direct contact with bodily fluids of infected people or with contaminated surfaces. People who contract Ebola require early detection and aggressive, high quality treatment. Timely, careful provision of rehydration treatments, management of accompanying symptoms—such as fever, bleeding or pain—and psychological support are critical aspects of care for patients with Ebola.
In March 2014, the Zaire ebolavirus surfaced in Guinea, and despite efforts to halt transmission, it quickly spread throughout West Africa, creating the largest Ebola epidemic to date. Nearly 30,000 cases were reported in Guinea, Liberia, Mali, Nigeria, Senegal and Sierra Leone, with over 11,000 resulting deaths.
Numerous factors contributed to the proliferation of the Ebola virus in West Africa, including environmental changes, ongoing conflict or other complex emergencies, depleted health systems and poverty. Fragile states, or settings in which the government is unable or unwilling to deliver basic security and public services to the majority of its people, are particularly vulnerable to infectious disease outbreaks. The negative impact of the Ebola epidemic was amplified in Sierra Leone in part due to the ongoing conflict and its weakened health system.
Consequences for maternal health
While Ebola is not a sex-specific virus, women and children suffered disproportionately from the outbreak. Pregnant women who contracted the virus were particularly vulnerable. Additionally, the closing of some health facilities during the epidemic and a shortage of health care providers able to properly diagnose and treat Ebola exacerbated existing health system challenges and reversed recent progress in access to maternal health care.
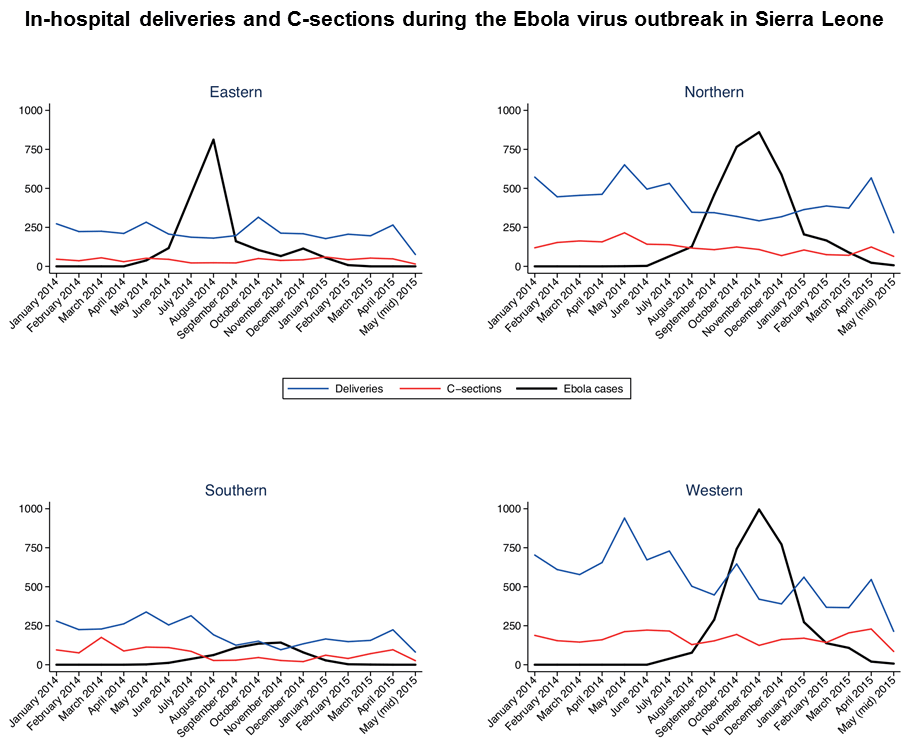
Even where services were available, however, fear of contracting the virus prevented many women from seeking care. Evidence indicated substantial decreases in facility-based delivery in Guinea, Liberia and Sierra Leone during the Ebola epidemic, as well as fewer antenatal care visits and cesarean section surgeries.
Source: Ribacke et al. The impact of the West Africa Ebola outbreak on obstetric health care in Sierra Leone. PLOS One, 2016.
Lasting impact on health systems
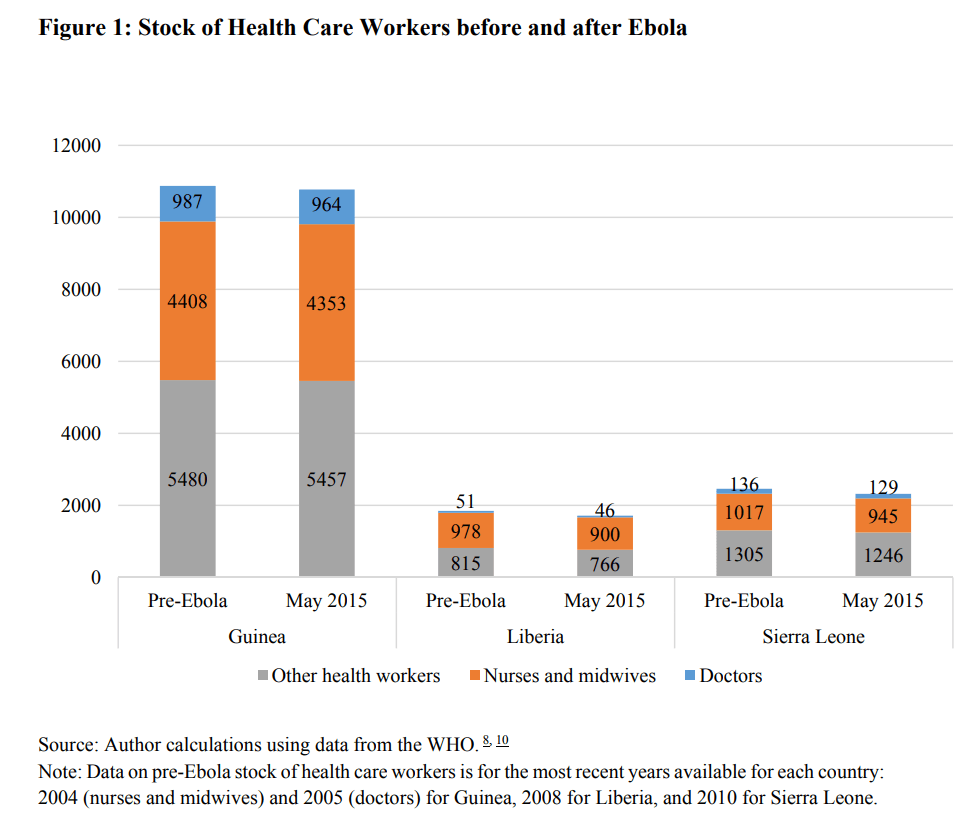
While the Ebola epidemic in West Africa officially ended in June 2016, it has had—and will likely continue to have—a lasting impact on maternal health in the region. Several doctors, nurses, midwives and other health care workers died while heroically treating people during the outbreak.
Source: Evans et al. The next wave of deaths from Ebola? The impact of health care worker mortality. 2015.
Community mistrust of health systems and personnel following the outbreak, as well as the collapse of health infrastructure, may help explain why utilization of essential maternal and child health services in Guinea remains lower than it was before March 2014. Women in the region also continue to face difficulties accessing contraceptives and family planning services.
Still, a lack of accurate data from different parts of the region before, during and after the outbreak hinders researchers’ ability to draw evidence-based conclusions and design and implement effective interventions. As such, Paul Spiegel, Director of the Johns Hopkins Center for Humanitarian Health, calls for a proactive approach to assessing interventions in the context of humanitarian settings:
“Maternal child health is an essential component of humanitarian preparedness and response. We need to collect better baseline information to allow us to study how effective the interventions are in each context. [We need] a special emphasis on implementation science – understanding better how to adapt specific interventions that have been shown to be effective in other settings to the unique and challenging humanitarian contexts.”
Efforts are needed to ensure that leaders, program implementers and researchers—especially those working in settings with limited resources—work collaboratively to prepare, prevent and manage future infectious disease outbreaks to minimize devastating effects on maternal health and health systems. As Omar Robles, Senior Program Officer, Adolescents in Emergencies at Women’s Refugee Commission, articulates, “Maternal health is a collective responsibility that necessitates collective action.”
—
Read [Part 3] Profiles of Maternal and Newborn Health in Humanitarian Settings: Conflict in Syria