In the past fifty years we have experienced incredible advances in health technology. In keeping with these technological advances, we see paradigm shifts in medical practice. Surgical procedures have shifted from open to laparoscopic to robotic. The prototype of limb prosthetics has shifted from appearance to function. Cancer treatment is experiencing a paradigm shift from historical chemotherapies to tumor targeted treatment and now targeted treatment of immune cells.
Not exempt from these technological advances is the field of obstetrics. Dating a pregnancy by conceptual age is more accurate, less confusing to today’s parent, and more appropriate for reproductive assistance. But, dating a pregnancy by conceptual age requires a higher level of technology. Gestational age dating is less specific but low-tech, low cost, low risk, and the generally accepted standard. What is perplexing is the general acceptance of a low-tech practice that is high risk. Research and advances in medical technology should move us out of these paradigms and into improved outcomes.
Safe reduction in the cesarean delivery has been a national priority. World-wide, obstetricians, midwives, and registered nurses vigilantly monitor fetal heart rates (FHR) knowing that the current practice of interpreting FHRs to deduce fetal oxygenation status, increases cesarean section rates, and does not necessarily improve neonatal outcome. These practitioners are pressured by institutions to keep primary cesarean section rates low while avoiding adverse outcomes, neonatal and legal. In real time novices and experts stress over menacing and reassuring fetal heart rate changes. Following expected and unexpected bad outcomes, expert practitioners and quality assurance councils review and rereview trying to determine what should have been done and when. Interpretation of fetal heart rate is taught in classrooms, at conferences, and at the bedside. But, no matter how invested we are academically and financially, it is time to move forward technologically.
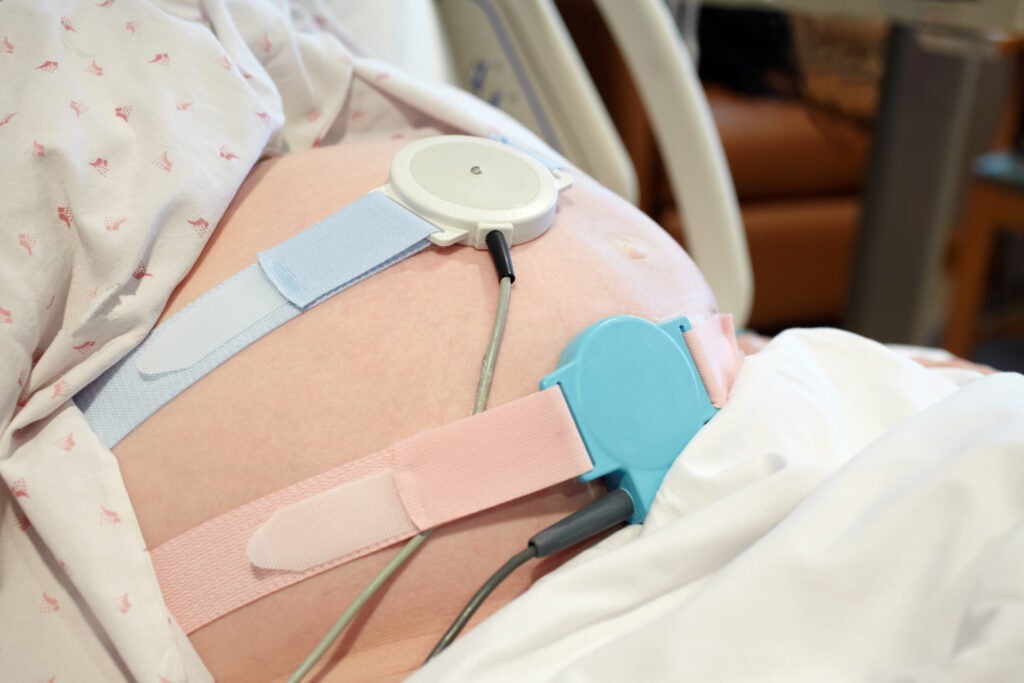
The physical act of maintaining a continuous fetal heart rate can be very labor intensive for nursing, particularly now with obesity affecting more than 30% of laboring women. Velcro, stockinette and even folded wash cloths are used to secure external monitors on pendulous abdomens or restless laborers. Efforts to improve external monitoring with new tools such as noninvasive detection of the fetal echocardiogram (fECG) and Maternal echocardiogram (mECG) rather than ultrasound doppler are still glitchy and only promote more of the same, interpreting a fetal heart rate pattern in order to assume well-being, hypoxia, or acidosis. Practitioners are still left with construing a measure versus realizing a measure.
When fetal scalp electrodes are applied, obviously more invasive, continuous monitoring is secure. Research in the 1980s and 1990s, investigated electrode techniques trying to find a biochemical method that could be used to monitor fetal wellbeing continuously, such as fetal tissue pH, fetal transcutaneous pO2, and pCO2 fetal base excess and fetal pulse oximetry. None of these methods are used today. Perhaps the idea of a biochemical method to monitor fetal wellbeing should be readdressed. In the 21st century we can identify cell-free DNA (cfDNA) in the maternal blood stream. Maternal blood can also be used to identify fetal red blood cells. The perceived cost of furthering this research, or alternative research, to assess real-time fetal well-being might be critically compared with the cost of maternal morbidity in the United States, approximately $32 billion. An Apple watch can detect extra-uterine oxygenation. Is there technology available to determine fetal oxygenation in real numbers so that we can shift the paradigm from predicting fetal hypoxia to diagnosing fetal hypoxia?
Electronic fetal monitoring (EFM), or cardiotocography, was developed more than fifty years ago. It was and is a subjective and imprecise method to predict fetal hypoxia in utero. For almost three quarters of a century we have analyzed, scrutinized, and questioned the value of electronic fetal monitoring. In 2017, research concluded that continuous electronic fetal monitoring resulted in no clear differences in cerebral palsy, infant mortality, or other standard measures of neonatal well-being. Yet, even the most recent research discusses improved interpretation. Can we stop researching methods to improve our guess and begin implementing diagnostic specificity for fetal hypoxia through modern technology?
In 2020, Tigchelaar et al published a clinical research article demonstrating success with a subcutaneous probe that could detect lactate levels in rats. Similar techniques are in use with diabetic patients for continuous glucose monitoring. In 2020, Ražem et al published a study that reported placental deoxygenation during labor, which is associated with fetal/neonatal acidosis, could be measured by noninvasive near-infra-red spectroscopy (NIRS). Although NIRS is increasingly adopted in different areas of medicine, studies regarding its potential use in obstetrics are rare.
Traditionally we have argued that research on pregnant women is too risky or unethical. In the least, research on pregnant women and unborn children is morally and ethically complex. However, we may have reached a point where not doing research may be more unethical. More and more international organizations and the American College of Obstetrics and Gynecology, and the Office of Research on Women’s Health of the National Institutes of Health encourage a paradigm shift from categorical exclusion to equitable inclusion in the research agenda. Pregnant women deserve equitable access to trials that result in direct benefit.
Imagine antepartum and intrapartum care with reduced cesarean section rates because the procedure only occurs when there is confirmed risk of fetal hypoxia and acidosis. Imagine a team of nurses, midwives, and physicians agreeing on exactly when and why to interrupt the labor process with an operative delivery. Imagine documenting actual fetal well-being instead of assumed fetal well-being. It is time to bring game changing research to obstetrics. It is time to relook and rethink how we practice intrapartum obstetrics; not more intervention, but better and smarter intervention, for laboring women.